Parkinson’s disease (PD), historically described as “Shaking Palsy,” is one of the most common neurological disorders affecting movement and coordination. It is a progressive neurodegenerative condition that develops gradually and requires long-term neurological care and management.
Parkinson’s disease is the second most common neurodegenerative disorder after dementia, yet with timely diagnosis and proper treatment, many patients continue to live active and independent lives for years.
Understanding Parkinson’s Disease
In simple terms, Parkinson’s disease can be compared to a clutch and gear malfunction in a vehicle. When the system responsible for smooth movement fails, speed and coordination are affected.
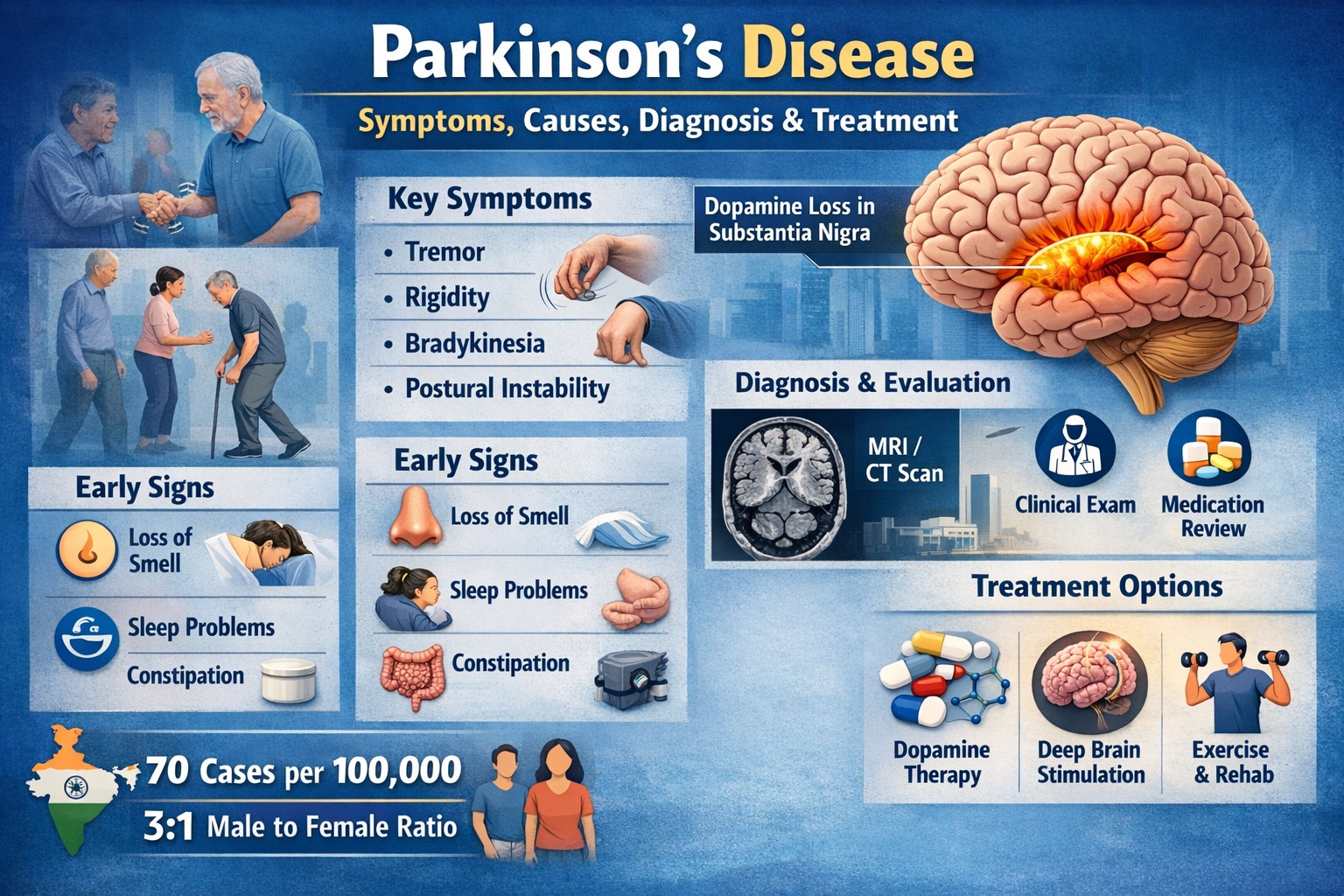
The brain requires dopamine, a neurotransmitter that acts like lubrication or “gear oil,” allowing smooth and controlled body movements. In Parkinson’s disease, nerve cells in a region of the brain called the substantia nigra gradually stop producing dopamine.
Symptoms usually appear only after 60–80% of dopamine-producing cells are lost.
What Happens in Parkinson’s Disease?
Loss of important neurotransmitters such as dopamine and norepinephrine leads to characteristic symptoms:
- Tremor – shaking of hands, legs, head, arms, or jaw
- Rigidity – stiffness of limbs and trunk
- Bradykinesia – slowness of movement
- Postural instability – impaired balance and tendency to fall
In common language, tremor is often mistaken as Parkinson’s disease, but tremor along with slowness and tendency to fall strongly suggests Parkinson’s disease.
Prevalence of Parkinson’s Disease in India
- India has one of the lowest reported incidence rates globally, approximately 70 cases per 100,000 population.
- Male gender is considered a significant risk factor.
- Male-to-female ratio ranges from 0.88 to 2.06.
Age-wise Male Predominance
- Age 40–49 years: Ratio ~ 3.11
- Age 50–59 years: Ratio ~ 3.29
- Age 60–69 years: Ratio ~ 2.03
- Age 70–72 years: Ratio ~ 2.30
Age of Onset
- Average onset age: Around 60 years
- Young Onset Parkinson’s Disease (YOPD): 21–40 years
- Juvenile Parkinsonism: Before 21 years
Less than 10% of cases are genetic and caused by single-gene disorders. Most cases are idiopathic, resulting from a complex interaction between genetic susceptibility and environmental factors.
Early Warning Signs (Non-Motor Symptoms)
Many patients experience symptoms years before movement problems begin. These early signs are often overlooked:
- Reduced sense of smell
- Chronic constipation
- Sleep disturbances (acting out dreams)
- Depression or anxiety
- Fatigue or mood changes
Recognizing these symptoms early can help in timely diagnosis.
Diagnosis of Parkinson’s Disease
Symptoms typically become noticeable 1–2 years after disease onset.
Diagnosis may sometimes be delayed because:
- About 25% of patients do not initially have tremors.
- Early symptoms may resemble other conditions.
Clinical Indicators Supporting Diagnosis
- Tremor with slowness of movement
- Tendency to fall
- Balance difficulties
Evaluation and Investigations
After clinical suspicion, doctors evaluate possible secondary causes of parkinsonism.
Medication Review
Certain medicines can worsen or mimic Parkinson’s symptoms:
- Antipsychotics (common in younger patients)
- Antiemetics
- Anti-epileptic medications
- Post-stroke conditions (more common in elderly)
Neuroimaging
Tests such as:
- CT Scan (Head)
- MRI Brain
are performed to rule out stroke, tumors, or structural abnormalities.
After excluding other causes, treatment with dopamine-based therapy is initiated.
Treatment of Parkinson’s Disease
Parkinson’s disease is manageable, and treatment aims to maintain independence and quality of life.
1. Dopamine Replacement Therapy (Main Treatment)
- Levodopa combinations
- Dopamine agonists
- Medication doses are carefully titrated according to patient needs.
Medication adjustment improves symptoms in nearly 80% of patients.
2. Surgical Treatment
In selected patients, especially:
- Young onset PD
- Juvenile Parkinsonism
Deep Brain Stimulation (DBS) may be considered at the appropriate stage.
3. Advanced Therapies (Emerging Options)
- Gene therapy
- Dopamine infusion therapy
- Neuroprotective treatments
- Disease-modifying therapies
These options are evolving and selected based on disease stage and patient condition.
Importance of Non-Drug Therapy
Lifestyle and rehabilitation therapies play a vital role in slowing functional decline:
- Regular exercise
- Physiotherapy
- Speech therapy
- Occupational therapy
These therapies improve mobility, balance, and independence.
Non-Motor Complications Over Time
As Parkinson’s progresses, patients may develop:
- Cognitive slowing or memory issues
- Depression or mood disorders
- Sleep disturbances
- Low blood pressure
- Constipation
- Bladder dysfunction
Regular follow-up helps doctors adjust treatment as symptoms change.
Role of Family Support
Family members play a crucial role in care by:
- Encouraging independence
- Ensuring home safety to prevent falls
- Monitoring mood and behavioral changes
- Supporting regular medical follow-ups
Living Well with Parkinson’s Disease
Although Parkinson’s disease is progressive, early diagnosis, proper medication, rehabilitation, and continuous neurological care allow many individuals to live productive and fulfilling lives for decades.
��⚕️ Expert Neurological Care
About Dr. Mukesh Kumar – Leading Neurologist in Delhi
Dr. Mukesh Kumar is among the most reputed and best neurologists in Delhi, widely recognized for his expertise in diagnosing and managing complex neurological conditions, including epilepsy and other brain disorders.
With more than two decades of excellence in neurology, he has developed strong clinical expertise in treating a wide range of neurological diseases. His vast experience reflects a deep commitment to providing effective, evidence-based neurological care through accurate diagnosis and advanced treatment strategies.
Dr. Mukesh Kumar stays updated with the latest medical and scientific advancements in disorders related to the central nervous system. His patient-centric approach focuses on understanding every individual’s condition in detail, ensuring that treatment plans are personalized, precise, and outcome-oriented.
His goal is not only to treat neurological disorders but also to improve patients’ quality of life through compassionate care, modern therapies, and long-term neurological management.